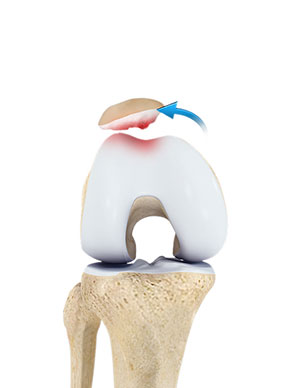
Patellofemoral pain syndrome (PFPS) is one of the most commonly reported knee problems, accounting for one in four knee complaints seen by orthopaedists.
Signs and symptoms
The signs and symptoms of patellofemoral pain syndrome can include the following:
- Pain in front of the knee, under and around the kneecap
- Increased pain while walking up or down the stairs
- Increased pain with kneeling and squatting
- Pain that worsens with activities and also occur with long bouts of inactivity
- Pain in one or both knees
- Pain that is usually described as “aching” but can also be “sharp” or “burning”
- A sensation that the knee may “give out”
- A grinding sensation that can be felt or heard when the knee is extended
- Swelling around the knee (rare)
Causes
Patellofemoral pain syndrome is caused by a multitude of factors that affect the way the patella moves along the groove of the femur (trochlear groove) when the leg is bent or straightened. The patella normally moves up and down with a slight tilt without touching the other knee bones. In PFPS, the patella rubs against the femur, causing pain.
A combination of factors can cause this abnormal tracking and include the following:
- Overuse/overload injury: Repeated weight bearing impact sports such as soccer and running can cause PFPS.
- Anatomical defect: Flat feet and high arches can cause misalignment of the knee joint.
- Weak quadriceps muscles: Quadriceps, the anterior thigh muscles, help hold the kneecap in place during movement. Weak thigh muscles can lead to abnormal tracking of the patella, causing it to rub against the femur, producing pain in the kneecap.
Risk factors
Anyone can develop patellofemoral pain at any point in their lives; however, there are certain risk factors that may predispose you to developing patellofemoral pain. These include:
- Starting a new physical activity
- Increasing the intensity of a physical activity too quickly
- Injury or trauma to the kneecap, which can lead to recurring episodes of instability
- Unusual alignment of the kneecap
- Arthritis
- Obesity
- Weak or tight thigh muscles
- Flat feet, knock knees or high arches
- Females are affected more than men as wider hips increase stress on the kneecap.
- Young athletes
Prevention
Although it may not always be possible to prevent patellofemoral pain syndrome, there are some measures you can take to decrease your risk.
These include:
- Appropriate warmup prior to an activity
- Alternating high impact activities with low impact activities
- Running on softer surfaces
- Gradually increasing the distance or intensity level
- Wearing proper footwear for your activity
- Strengthening your quadriceps to prevent abnormal tracking of the patella
- Stopping the activity when symptoms of PFPS occur with a gradual return once symptoms improve
Diagnosis
Identifying the source of patellofemoral pain is critical in determining your treatment options for pain relief.
Your physician will review your
- Medical history and perform a thorough
- Physical examination.
Your doctor may order X-rays, CT scan and MRI scan to determine the cause of your knee pain and rule out other conditions.
Treatment Options
Treatment for patellofemoral pain will depend on the exact cause of the pain and whether the pain is acute or chronic.
Treatment options for acute PFPS include:
Pain medications
Over-the-counter NSAIDs (nonsteroidal anti-inflammatory drugs) can help with the pain and any swelling.
Rest
Stay off the injured knee as much as possible and avoid activities that can cause pain, as more damage could result from putting pressure on the injury. You can perform non-weight bearing activities such as swimming. Slow, gradual resumption of activities is advised.
Ice
Ice packs applied to the injury will help reduce swelling and pain. Ice should be applied over a towel to the affected area for 20 minutes every hour. Never place ice directly over the skin.Treatment options for chronic PFPS include:
If your knee pain persists despite the above treatments, your doctor may suggest more intensive treatments. These may include the following:
Physiotherapy
PT can teach you the proper stretching and strengthening exercises appropriate for your condition. Working on the quadriceps (thigh muscles) is a primary focus for treatment of PFPS. If the cause of your knee pain is a different muscle group, such as hamstrings, your therapist will individualise your exercises accordingly.
Bracing
Soft braces with cut-outs over the patella may be suggested for support and alignment.
Taping
Your therapist may show you how to tape the knee to bring it into proper alignment.
Orthotics
Shoe inserts may be ordered when PFPS is caused by foot abnormalities, such as flat feet.
Surgery
Although uncommon, surgical treatment is sometimes necessary to help relieve the pain if your PFPS persists and does not respond to conservative treatment. Your surgeon may recommend arthroscopy to evaluate your condition and repair or remove any fragmented cartilage.
