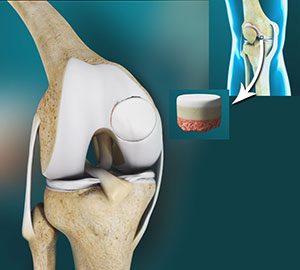
What is an Osteochondral allograft?
Osteochondral grafting is a method of treating cartilage injuries that expose the underlying bone. An osteochondral allograft is a piece of tissue containing bone and cartilage that is taken from a deceased donor to replace damaged cartilage that lines the ends of bones in a joint. The allograft tissue is shaped to precisely fit the defect in the damaged joint of the patient and then transplanted to repair the damage.
Anatomy
The articulating surfaces of all joints in the body are lined by a soft tissue called articular cartilage, which cushions the ends of bones. This allows easy gliding of the bones during movement of the joint. Injury and wear-and-tear can damage the cartilage, making it rough and exposing the underlying bone. This leads to painful rubbing of the bones of the joint and disability.
When is Osteochondral grafting indicated?
- Osteochondral grafting is indicated for:
- Large areas of damage with the diameter ranging from 15 to 35 mm
- Symptoms of pain, swelling, and catching
- Localized, full-thickness injuries
- Patients under 50 years of age
- Active patients with high physical demand
- Osteochondritis dissecans (lack of blood supply separates a segment of bone from its surrounding)
- Avascular necrosis (death of bone tissue)
Surgical Procedure for Implantation of an Osteochondral Allograft
The implantation of osteochondral allografts is usually performed through an open incision, under general or spinal anesthesia. An incision is made to expose the joint defect. The size of the defect is then measured, and a portion of the cartilage and underlying bone is removed.
A fresh allograft taken from a deceased donor is sterilized, prepared in the laboratory and tested for risk of disease transmission. It is then trimmed with an oscillating saw to match the size of the prepared defect. The allograft is then gently press-fit into the defect created in the recipient's bone. It can be further stabilized with metallic screws and pins if needed. The incision is then closed, and a dressing applied to the joint.
Post-operative Care
Following the surgery, a brace may be applied for the first 2 weeks. Your surgeon will prescribe medication to reduce pain. You will be instructed to use crutches and limit bearing weight for 6 to 8 weeks. Early movement is encouraged, and you will be gradually introduced to physical therapy, which will be continued for 8 to 12 weeks.
You may be able to return fully to your activities in 6 to 12 months.
Advantages & Disadvantages of Using Allografts
When compared to osteochondral autografts (tissue is taken from another part of your own body), osteochondral allografts can help reconstruct larger three-dimensional articular defects without incurring defects at the donor site. They are specifically indicated for young, active patients with larger lesions.
However, osteochondral allografts are associated with a higher risk of immune-mediated graft rejection and disease transmission from the deceased donor. Another disadvantage includes low availability as it may be difficult to obtain fresh donor specimens with the required cartilage thickness.
Risks and Complications of Osteochondral Allografts
As with all surgical procedures, the transplantation of osteochondral allografts may be associated with certain risks and complications such as:
- Infection
- Pain
- Bleeding
- Implant failure
- Joint Stiffness
- Blood clots
Related Topics
- Total Knee Replacement
- Revision Knee Replacement
- Uni Knee Replacement
- Knee Arthroscopy
- Medial Collateral Ligament Reconstruction
- ACL Reconstruction Using Hamstring Tendon
- Cartilage Grafting
- Matrix-induced Chondrocyte Implantation
- Osteochondral Allograft
- Osteochondral Autograft
- Microfracture
- Intra-articular Knee Injections
- Knee Rehabilitation
